What Are Varicose Vein Treatment Insurance Policy Limitations In New York?
It’s crucial to understand that not all treatments for varicose veins are reimbursed by insurance. In order to help you make educated decisions about your healthcare and tell you What kind of doctor specializes in veins, this article will describe the insurance constraints for varicose vein treatments.
Varicose Vein Treatment Options
Compression Stockings
The first step in treating varicose veins is frequently wearing compression stockings. They are special stockings or socks that aid in enhancing blood circulation in your legs. Even though they can be helpful in easing pain and keeping the illness from getting worse, insurance may not always cover them unless a doctor prescribes them.
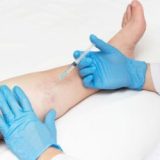
Sclerotherapy
A specific solution is injected into the afflicted veins during the minimally invasive treatment known as sclerotherapy. The vein gradually dissipates and collapses as a result of this solution. When sclerotherapy is deemed medically necessary, such as when varicose veins cause discomfort or other issues, it is typically covered by insurance.
Endovenous Laser Treatment (EVLT) or Radiofrequency Ablation (RFA)
Modern procedures like EVLT and RFA use heat to seal off troublesome veins. When there is a proven medical necessity, such as substantial pain, swelling, or skin changes as a result of varicose veins, these procedures are often reimbursed by insurance.
Policy Limitations for Varicose Vein Treatments
Medical Necessity
For most insurance policies, coverage of a therapy requires that it be declared medically essential. This means that for the treatment to be considered, you must have particular symptoms or complications related to your varicose veins. Insurance is unlikely to pay for treatment if your main goal is cosmetic.
In-Network Providers
Networks of healthcare providers with whom insurance companies have negotiated rates are common. Treatment for varicose veins received from an out-of-network practitioner may incur greater out-of-pocket expenses or could result in no coverage at all. To discover local in-network providers, contact your insurance carrier.
Deductibles and Copayments
You can still be required to pay deductibles and copayments even if your insurance covers varicose vein therapy. Copayments are a portion of the overall cost that you are liable for, whereas deductibles are a fixed amount that you must pay before your insurance begins to pay. To prevent unforeseen costs, be sure to comprehend the conditions of your insurance coverage.
Coverage Limits
Some insurance policies place restrictions on the number of treatments or the overall cost of varicose vein procedures that they will pay for. Reviewing your policy documents is essential to see whether any such restrictions are set down therein.
Pre-Existing Condition Clauses
You should be aware of any pre-existing condition clauses if you have varicose veins before getting your current insurance coverage. For a predetermined waiting time, some policies may not pay for treatments for ailments that existed before your coverage started.
Conclusion
In conclusion, you now know ‘Are Varicose Vein Treatments Covered‘ by Insurance and why it is crucial to comprehend the policy restrictions on varicose vein treatments in order to make wise healthcare judgments. It’s important to study the conditions of your individual plan and, if necessary, contact your insurance provider for clarification because insurance coverage differs from policy to policy. Knowing your insurance coverage can help you explore the treatment options that are accessible to you while efficiently managing the related expenditures, even if varicose veins can be a source of agony and worry. Always get advice from your healthcare practitioner and insurance provider to be sure you’re making the best decisions possible for your particular circumstances.