Do Insurance Providers Identify Varicose Vein Treatments as Medically Necessary?
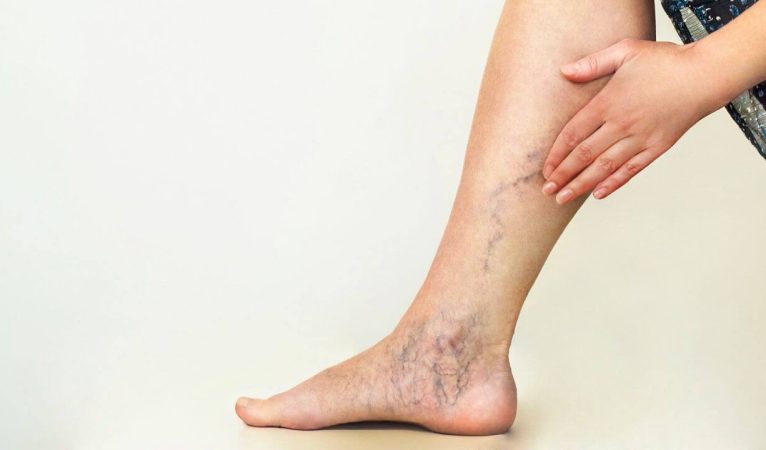
Large, twisted veins called varicose veins can be uncomfortable and adversely affect our legs’ appearance. Many people are curious about Are varicose veins covered by insurance? as medically required and whether they are covered by insurance.
What Are The Elements Affecting Insurance Coverage?
Medical Needs Standards
When considering whether to fund varicose vein treatments, insurance providers often consider a medical necessity. Treatment must be medically necessary to treat a medical issue that harms your health and well-being. Specific requirements must be completed in order for varicose vein treatments to be justified as medically essential. These requirements could include the presence of varicose vein-related symptoms such as leg pain, swelling, cramping, or skin abnormalities.
Precautionary Actions
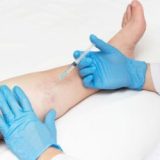
Insurance companies can require consumers to first try preventative measures before accepting payment for varicose vein procedures. Conservative approaches refer to non-invasive or less expensive procedures to cure symptoms and control varicose veins. Wearing compression stockings, elevating the legs, exercising frequently, or taking over-the-counter painkillers are a few examples of these approaches. Further therapies might be covered by insurance if conservative approaches are ineffective in providing enough relief.
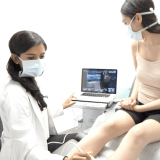
Ultrasound Assessment
In order to evaluate the severity of varicose veins and choose the best course of action, insurance providers could demand an ultrasound examination. Venous reflux, a disease in which blood flows backward in the veins and results in varicose veins, can be located, and its extent can be determined with ultrasound. Insurance companies may use this assessment’s findings to decide whether varicose vein treatments are medically essential.
Effects On Function And Symptoms
Insurance coverage for varicose vein treatments depends critically on the presence of symptoms and functional impairment. In the event that varicose veins are seriously uncomfortable or impair daily activities, employment, or mobility, the treatments may be deemed medically required. For instance, insurance companies may be more inclined to pay for treatments if varicose veins make it difficult for a person to stand or walk for long periods of time.
Considerations For Beauty
It’s crucial to know that insurance companies frequently make a difference between treatments for varicose veins performed for cosmetic versus medical reasons. Treatments undertaken solely for aesthetic purposes as opposed to resolving medical conditions are referred to as cosmetic procedures. In general, insurance companies don’t pay for varicose vein treatments that are just done for aesthetic reasons. However, insurers may view the procedures as medically essential if varicose veins result in pain, discomfort, or functional impairment.
In Conclusion
Various criteria determine whether insurance companies view varicose vein treatments as medically necessary. In most cases, how much does varicose vein treatment cost?, symptoms, functional impairment, and the failure of conservative efforts to reduce pain are the criteria for insurance reimbursement for these treatments. An ultrasound examination may also be needed to determine the degree of varicose veins. It is critical to speak with a vascular specialist and confirm with your insurance company whether varicose vein treatments are covered in your situation. Do not forget that treating your varicose veins can enhance your quality of life and improve vascular health in the long run.